Support when
you need it

Support when
you need it
IPSEN CARES™
Helping patients get access to their prescribed medications with the information and support they need.
IPSEN CARES (Coverage, Access, Reimbursement & Education Support) serves as a central point of contact between patients/caregivers, healthcare providers (HCPs), insurance companies, and specialty pharmacies.

Patient support for eligible* and enrolled patients prescribed Dysport®
Once the provider has prescribed Dysport for injection,
the IPSEN CARES Patient Access Managers are fully dedicated to:
- Facilitating patients’ access to their prescribed medications
- Providing information and support for the interactions among offices, patients, and insurance companies for Ipsen medications

IPSEN CARES Enrollment Is Quick and Easy
Patients must be enrolled to access all IPSEN CARES support offerings.
- Patient and HCP download the IPSEN CARES Enrollment Form and complete it at the office. The form is submitted electronically or by printing and faxing it to IPSEN CARES.
- Once a completed Enrollment Form is received, an IPSEN CARES Patient Access Manager will conduct a benefits verification to review the patient’s out-of-pocket costs associated with Dysport. Additional support offerings for which the patient may be eligible will be discussed at that time.
![]()
Patient Authorization
Patients/caregivers are required to sign the Dysport Patient Authorization Form every 3 years, or sooner if required by state law, to give the Patient Access Specialists at IPSEN CARES permission to access the patient’s personal health information in order to help with treatment. The form can be signed and submitted online, or by downloadable PDF, which must be printed, filled out, signed, and faxed.

Copay Assistance
With the Dysport Copay Assistance Program, you may pay as little as $0 for each Dysport prescription. Here is the key information and eligibility* criteria:
- You currently have commercial (private) health insurance that covers Dysport
- You also have no primary or secondary insurance coverage under any state or federal healthcare program
- You have US residency
- You have a valid prescription for Dysport
*Visit ipsencares.com for full Patient Eligibility and Terms & Conditions.
To learn more about IPSEN CARES, visit www.ipsencares.com or contact directly.
Phone: 1-866-435-5677 Fax: 1-888-525-2416 Hours: 8 am - 8 pm ET Monday-Friday
National Dysport Coverage Overview*
For Patients With Spasticity and Adult Cervical Dystonia, Dysport Has National Coverage Without Restrictions
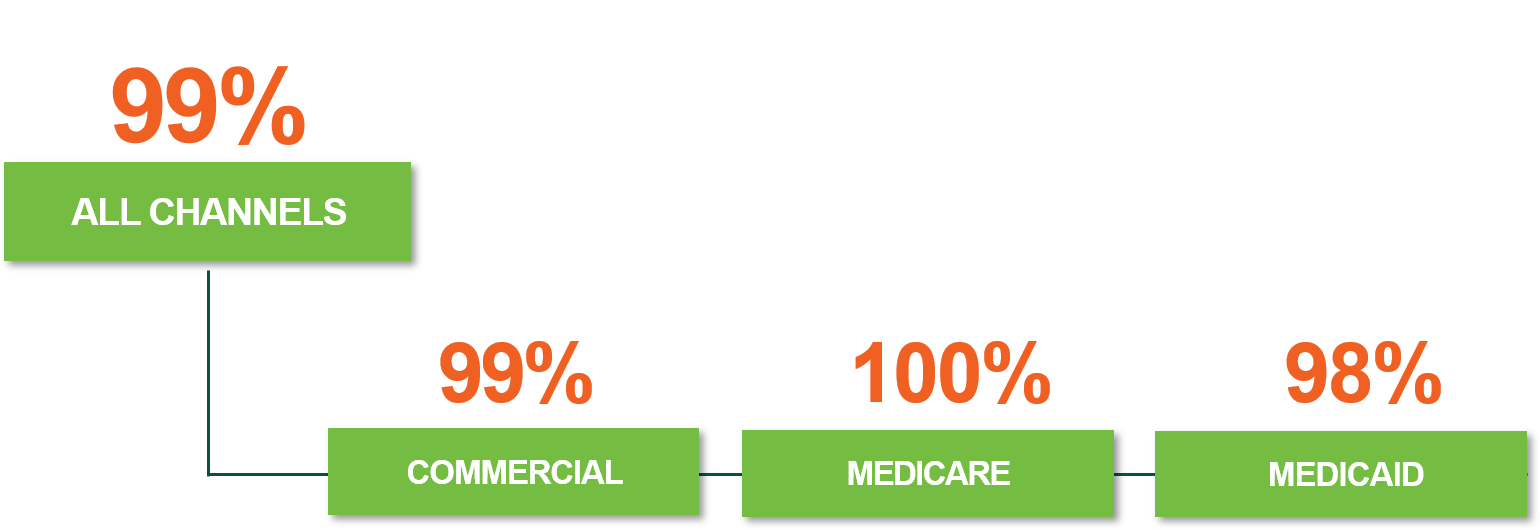
*Data provided by Breakaway Partners Essentials and current as of August 2023
Includes Managed and State Medicaid
Additional Support
Support from those who understand your condition,
because you’re not alone.
Support from those who understand your condition,
because you’re not alone.
The spasticity community: Connect with others in similar situations for support, information, or just to have an understanding friend. Sometimes, people who don’t have a child with spasticity just aren’t able to understand what it feels like. Remind yourself that you and your child are not alone and can reach out. Through these organizations, you and your whole family can find helpful information about living with spasticity.
Information about patient advocacy groups is provided for convenience and does not imply an endorsement of these organizations by Ipsen or by these organizations of Ipsen.









